Navigating through the later stages of life, women encounter a significant milestone known as menopause. This natural transition often occurs in a woman’s late 40s to early 50s but can present itself uniquely for each individual.
Understanding the signs and symptoms becomes crucial for managing this phase with grace and well-being as the body begins to signal the end of reproductive years.
Menopause comes with its own set of signals, such as unpredictable periods, intense hot flashes, night sweats, swings in mood, and shifts in sexual interest. These signs are the body’s way of adapting to lower levels of estrogen and progesterone.
This phase often challenges women both physically and emotionally, prompting the need for reliable treatments. Thankfully, healthcare has evolved, offering several ways to ease these symptoms. Options include hormone replacement therapy (HRT) and making changes in daily habits to improve overall well-being.
This article delves into the nuances of menopause among seniors, offering insights into recognizing symptoms and exploring the available treatments to navigate this chapter confidently.
Everything You Need to Know About Menopause
Understanding the changes that occur during menopause and perimenopause is crucial. It’s important to prepare for the physical and emotional effects that they can have on a woman’s life. By being informed about this phase and recognizing the signs, women can receive appropriate medical guidance and discover effective ways to manage their symptoms.
Prefer to listen rather than read?
Menopause also brings a hike in the risk of osteoporosis, heart disease, and urinary incontinence. By understanding these risks, women can get ahead of them. Actions like keeping active, eating right, and talking over prevention with their doctor can make a big difference.
Understanding menopause and perimenopause is crucial for women, as it can help them prepare for the changes that are coming and manage the symptoms that may arise. Navigating this transition with knowledge and confidence can also help women maintain their overall health and well-being.
This post will cover tips and insights on how to navigate menopause and perimenopause, including lifestyle changes, hormone therapy options, alternative treatments, the importance of education and understanding, personal experiences and perspectives, and common misconceptions.
Perimenopause Period
Let’s dive into the topic of the Perimenopause Period. This phase marks a transition towards menopause, signaling the winding down of a woman’s reproductive years. It’s a change that usually kicks off in the 40s, though it can start earlier or later. This phase stretches out for several years until menopause officially begins. During this time, a woman’s ovaries dial back on estrogen production, leading to irregular or sometimes heavier periods than before.
Feeling hot, sweaty, moody, dry down there, and less interested in sex? Perimenopause is a natural aging process that can cause some common symptoms. Talk to your doctor if you’re experiencing any of these symptoms. There are many treatment options available to help you manage these symptoms and improve your quality of life during this transition.

Common Signs and Symptoms
Although every woman’s experience is unique, most will experience common signs and symptoms of menopause. These symptoms can be both physical and emotional, and they can affect a woman’s daily life. It is important to gain knowledge about these symptoms, as understanding what to expect can help women navigate this transition with greater ease.
These are the most common ones include:
Irregular Periods
- One of the most common changes in menstrual patterns during menopause is irregular periods.
- As a woman approaches menopause, her ovaries produce less estrogen and progesterone, the hormones that regulate the menstrual cycle.
- This can cause periods to become irregular, with longer or shorter cycles, heavier or lighter bleeding, or even missed periods.
- Some women may experience spotting or light bleeding in between periods, which can be concerning.
- However, this is usually a normal part of the menopause transition, as hormonal changes can cause irregular bleeding.
- Women experiencing this should still talk to their healthcare provider if they experience any unexpected bleeding, as it could also be a sign of other medical conditions.
Hot Flashes
- Hot flashes are one of the most common symptoms of menopause, affecting up to 80% of women during the transition.
- They are caused by hormonal changes that disrupt the body’s temperature regulation system, leading to a sudden feeling of warmth that can spread from the chest to the neck, face, and arms.
- This is often accompanied by sweating and flushing of the skin.
- Hot flashes can last from a few seconds to several minutes and can occur several times a day or a few times a week.
- They can be mild or severe, and some women may experience them for several years after menopause.

Night Sweats
- Night sweats are a common symptom experienced by women during the menopausal transition, affecting up to 75% of women.
- They occur in the form of sudden, intense heat that can cause sweating and discomfort, and are usually accompanied by fatigue, irritability, and anxiety.
- Night sweats are similar to hot flashes, but they occur during sleep and can cause women to wake up feeling damp or wet.
- The exact cause of night sweats during menopause is not fully understood, but it is thought to be related to hormonal changes in the body.
- As estrogen levels decline, the hypothalamus, which regulates body temperature, becomes confused and sends signals to the body to cool down.
- This leads to a sudden rise in body temperature, followed by sweating and flushing.
Vaginal dryness
- As estrogen levels decline during menopause, the vaginal tissues can become thinner, drier, and less elastic.
- This is known as vaginal atrophy or genitourinary syndrome of menopause (GSM), and it can cause a range of uncomfortable symptoms, including vaginal dryness, itching, burning, and pain during sex.
- Vaginal atrophy can also lead to an increased risk of vaginal and urinary tract infections, as the thinning and drying of the tissues can make it easier for bacteria to grow.
Mood Changes
- It can cause a range of emotional and psychological symptoms, including mood swings, irritability, anxiety, and depression, in some women.
- The hormonal changes that occur during menopause can affect the levels of neurotransmitters in the brain, such as serotonin and dopamine, which can contribute to mood changes and depression.
- It can be a stressful and challenging time for many women, as they may be dealing with a range of physical and emotional changes, as well as life transitions such as children leaving home or retirement.
Sleep disturbances
- Insomnia or other sleep disturbances are commonly experienced by women during menopause.
- This is often due to the hormonal changes that occur during this time, which can lead to hot flashes and night sweats that disrupt sleep.
- While these symptoms may vary in severity and frequency among women, they can significantly impact a woman’s quality of life and overall health.
Changes in Libido
- Some women may experience a decrease in sex drive or difficulty achieving orgasm during menopause.
- The hormonal changes that occur during menopause can affect sexual function in several ways.
- For example, the decrease in estrogen levels can cause a decrease in blood flow to the genital area, leading to vaginal dryness and discomfort during sex.
- This can make sex less pleasurable and may contribute to a decrease in sexual desire.
- The decrease in testosterone levels that occurs during menopause can also contribute to a decrease in sex drive or difficulty achieving orgasm. Testosterone is an important hormone for sexual function in both men and women, and its decline during menopause can affect sexual desire and response.

Urinary Problems
- The loss of estrogen during menopause can cause changes in the urinary tract, leading to urinary incontinence, frequent urination, or urinary tract infections.
- Estrogen helps to maintain the health and elasticity of the tissues in the urinary tract, including the urethra, bladder, and ureter.
- As estrogen levels decline during menopause, these tissues may become thinner and weaker, leading to urinary problems.
- Urinary incontinence is a common problem experienced by women during menopause, particularly stress incontinence, which occurs when physical activity or pressure on the bladder causes urine to leak.
- This can be caused by the weakening of the pelvic floor muscles, which support the bladder and urethra.
- Frequent urination is also a common problem during menopause, particularly during the nighttime.
- This can be caused by a decrease in the bladder’s ability to hold urine or a decrease in the production of the hormone vasopressin, which helps regulate urine production during sleep.
- Urinary tract infections are also more common during menopause due to changes in the urinary tract’s bacterial environment and the thinning of the tissues, which can make it easier for bacteria to enter the bladder or urethra.
It is worth emphasizing that every woman’s experience of menopause is unique, and not all women encounter all of the symptoms outlined. The severity and duration of these symptoms can differ substantially as well. If you are experiencing any of these symptoms, it is advisable to seek advice and assistance from your healthcare provider for proper guidance and support.
What are the Treatment Options
Menopause is a natural part of a woman’s life, but the symptoms that come with it can be quite challenging to deal with. The good news is that there are several treatment options available that can make this transition a lot smoother. While some women may be hesitant to seek treatment, they should consider it. There are several treatment options available for menopause, depending on the individual’s symptoms and overall health.
Here are some of the most common treatments:
Hormone Therapy (HT)
- Hormone therapy is a treatment that replaces the estrogen and progesterone hormones that are lost during menopause.
- It can help relieve symptoms such as hot flashes, night sweats, vaginal dryness, and mood swings.
- Hormone therapy can be taken in the form of pills, patches, creams, gels, or vaginal rings.
- However, it is important to note that hormone therapy is not suitable for everyone, and it may increase the risk of certain health conditions such as breast cancer, stroke, and blood clots.
Non-Hormonal Treatments
- Non-hormonal treatments such as antidepressants, anti-seizure medications, and blood pressure medications have been found to be effective in relieving symptoms such as hot flashes and mood swings during menopause.
- These medications work by affecting the levels of certain neurotransmitters or chemicals in the brain that are involved in regulating mood, sleep, and other functions.
- However, it is important to note that these medications may have potential side effects and should only be taken under the guidance of a healthcare provider.
Vaginal Estrogen
- Vaginal estrogen is a type of hormone therapy that is specifically designed to treat vaginal dryness and discomfort during sex. It is most commonly used by women who are going through menopause, as this is a time when the body’s natural estrogen levels decrease, leading to a range of symptoms, including vaginal dryness.
- Vaginal estrogen comes in several different forms, including creams, tablets, and vaginal rings. Creams are typically applied to the vaginal area using an applicator, while tablets are inserted into the vagina in a similar way. Vaginal rings are small, flexible devices that are placed inside the vagina, where they slowly release estrogen over time.
- These different forms of vaginal estrogen work in slightly different ways, but they all help to increase estrogen levels in the vaginal tissue, which can help to relieve symptoms such as dryness, itching, and discomfort during sex. This can have a significant impact on a woman’s quality of life, allowing her to enjoy a more comfortable and fulfilling sexual experience.
- While vaginal estrogen is generally considered safe and effective, it is important to talk to a healthcare provider before starting any new medication or hormone therapy. This is especially true for women who have a history of breast cancer, as estrogen can sometimes promote the growth of certain types of breast cancer cells. However, for most women, vaginal estrogen is a safe and effective option for managing the symptoms of vaginal dryness and discomfort. In regards to breast cancer, early detection is always a viable option.
Lifestyle Changes
- One of the most effective ways to manage hot flashes is by avoiding triggers that can make them worse. Some common triggers include caffeine, alcohol, spicy foods, and hot drinks. By avoiding these triggers, women can reduce the frequency and severity of their hot flashes.
- Staying cool is another important strategy for managing hot flashes. This can involve wearing lightweight, breathable clothing, using a fan or air conditioning to keep the room cool, and drinking plenty of cool water to stay hydrated.
- Practising relaxation techniques such as deep breathing, meditation, and yoga can also be helpful for managing hot flashes. These techniques can help to reduce stress and anxiety, which can exacerbate hot flashes.
- For women who are experiencing severe hot flashes, hormone therapy or other medications may be recommended by a healthcare provider. Hormone therapy involves taking estrogen and progesterone, which can help to regulate hormone levels and reduce the frequency and severity of hot flashes. However, hormone therapy is not suitable for everyone and may carry some risks, so it is important to discuss this option with a healthcare provider.
Alternative Therapies
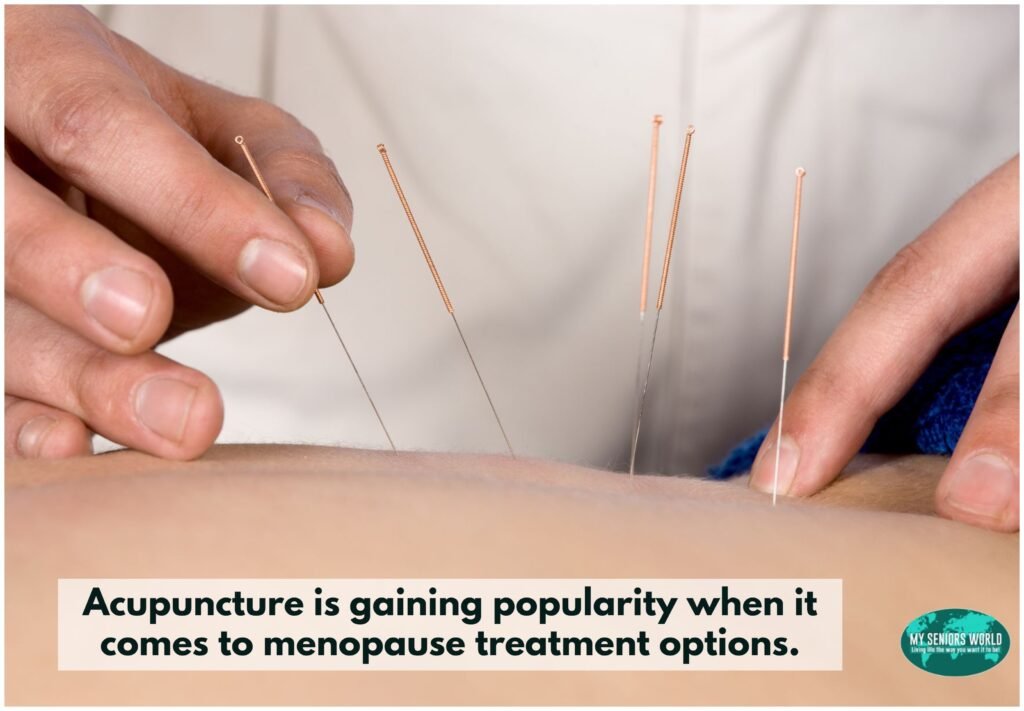
- Alternative therapies such as acupuncture, herbal supplements, and yoga have been gaining popularity as natural approaches to managing menopause symptoms. While some women may find relief from these therapies, it is important to remember that they may not work for everyone, and some may have potential risks or interactions with other medications.
- The practice of acupuncture, which is rooted in traditional Chinese medicine, entails the insertion of slender needles into precise points on the body. While certain studies have indicated that acupuncture may be helpful in decreasing hot flashes, night sweats, and other symptoms associated with menopause, additional research is required to gain a complete understanding of its effectiveness. Consequently, it is critical to locate a licensed acupuncturist who has expertise in treating menopause symptoms.
- Herbal supplements are another alternative therapy that some women turn to for menopause symptom relief. Supplements such as black cohosh, soy, and red clover have been used to help manage hot flashes, mood changes, and vaginal dryness. However, it is important to note that herbal supplements are not regulated by the FDA and may have potential side effects or interactions with other medications. It is important to talk to a healthcare provider before taking any herbal supplements for menopause symptoms.
- Yoga and other mind-body practices such as meditation and tai chi have been shown to reduce stress and improve overall well-being, which may help to manage menopause symptoms. Yoga, in particular, has been shown to improve sleep, reduce hot flashes, and increase feelings of well-being in women going through menopause. However, it is important to find a qualified yoga instructor who has experience working with menopausal women, as certain poses may not be appropriate or comfortable for everyone.
It’s important to remember that the treatment options for menopause vary depending on individual needs and preferences, and not all options may be suitable for everyone. It’s important to consult with a healthcare provider to determine the best treatment plan for your individual needs.
Conclusion
In conclusion, menopause can be a challenging time for women, with a variety of physical and emotional symptoms that can impact their daily lives. However, with the right information and support, women can navigate this time with confidence and minimize the negative effects of menopause. This post can be an invaluable resource for women looking to learn more about menopause and how to manage their symptoms.
By staying informed and working closely with their healthcare provider, women can take control of their health and well-being during this important stage of life.
Disclaimer
The content provided on MySeniors.World is for informational purposes only and is not intended as either financial or medical advice. Always consult a qualified professional before making any investment or health-related decisions.
Posts may contain affiliate links, meaning we earn a commission – at no additional cost to you, if you click through and make a purchase. Your support helps us continue providing valuable content.



















