Parkinson’s disease is a challenge, no two ways about it. For seniors who’ve been diagnosed, it might feel like a massive curveball has been thrown their way. But remember, life isn’t about waiting for the storm to pass but learning to dance in the rain. And for caregivers, supporting someone with Parkinson’s is a journey of compassion, understanding, and patience.
When we say Parkinson’s, we’re talking about a progressive neurological disorder that affects movement. It’s a result of certain nerve cells in the brain not producing enough of a chemical called dopamine.
Everything You Need to Know About Parkinson’s
Parkinson’s disease, a debilitating neurodegenerative disorder, exerts its devastating effects primarily on movement. This chronic condition takes its toll on individuals when a significant number of dopamine-producing cells in the brain start to dwindle.
The gradual decline of these cells marks the onset of a multitude of distressing symptoms that relentlessly progress over time, shaping the lives of older people afflicted by this cruel illness. Dopamine, a vital neurotransmitter responsible for transmitting signals between nerve cells, plays a crucial role in regulating movement and coordination.
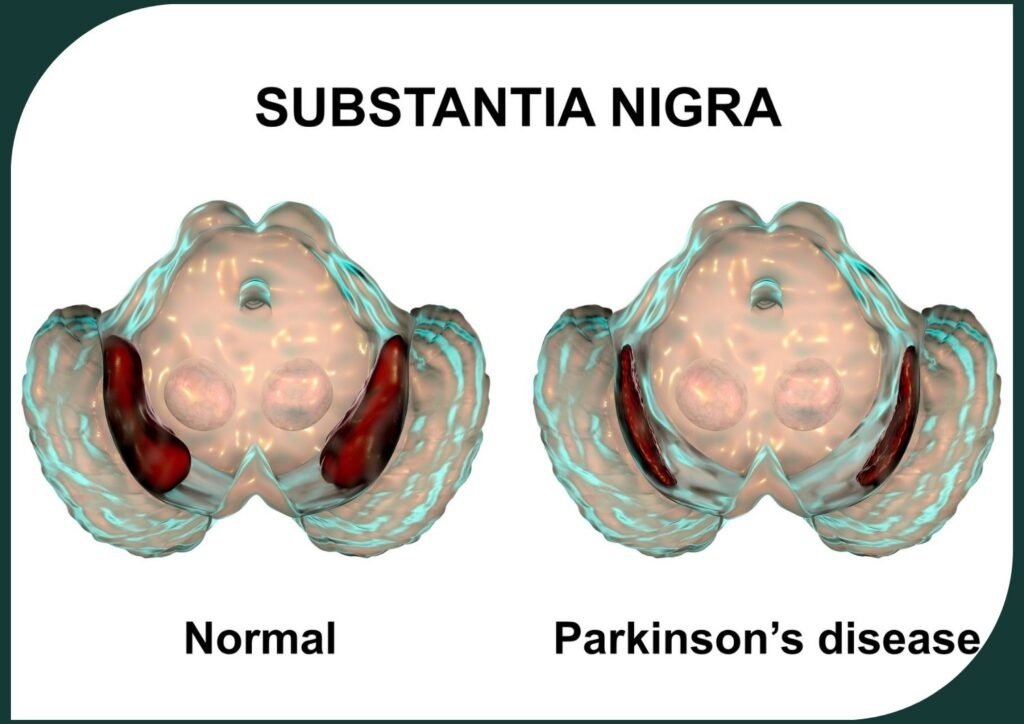
However, in Parkinson’s disease, the insidious destruction of dopamine-producing cells in an area of the brain called the substantia nigra disrupts this delicate balance. This depletion of dopamine leads to an imbalance in the brain’s communication pathways, ultimately resulting in the hallmark motor symptoms of Parkinson’s disease.
Prefer to listen rather than read?
The Subtle Onset of Symptoms
Parkinson’s disease typically begins with subtle symptoms that may be mistaken for signs of aging or stress. These early signs often go unnoticed, but they are crucial in early diagnosis and intervention. Common early symptoms include:
Tremors
One of the most well-known symptoms of Parkinson’s is resting tremors, typically occurring in the hands, fingers, and sometimes the chin or lip. These tremors are often more pronounced when at rest.
You might notice this as shaking in the hands, fingers, or even the chin and lip, especially when the person is relaxed or not moving. Such tremors can make daily tasks a bit tricky, but understanding them is the first step towards managing them effectively.

Bradykinesia
Bradykinesia, a hallmark of Parkinson’s, describes the frustrating slowness in motion. Those living with it often encounter a gradual decline in their capacity to start and finish tasks, turning once-simple activities into time-consuming challenges. This gradual reduction in movement speed can significantly impact their daily lives.
Muscle Stiffness
Muscle stiffness, or rigidity, is a frequent symptom of Parkinson’s disease. This condition can impact different muscle groups, resulting in discomfort and limiting one’s ability to move comfortably. This stiffness can be quite bothersome, making it essential for those affected to seek appropriate care and support for enhanced well-being.

Postural Instability
Patients may discover that maintaining an upright posture becomes progressively difficult, resulting in balance issues and a heightened risk of falls. This physical challenge can significantly impact their daily lives, making it essential to seek expert guidance and support to regain stability and confidence.
Advanced Symptoms
As Parkinson’s disease progresses, so do its symptoms. Patients may experience a broad range of both motor and non-motor issues. It’s crucial to be aware of these advanced symptoms to provide the best possible care:
Freezing of Gait
It is an abrupt, but brief, episode where one’s feet seem glued to the ground, despite the strong desire to take a step. This phenomenon can have serious consequences, such as unexpected falls and injuries.
It’s a puzzling challenge that many individuals with Parkinson’s face, highlighting the need for expert guidance and support in managing this complex condition.
Speech and Swallowing Difficulties
Parkinson’s disease can impact the muscles crucial for speech and swallowing, potentially causing slurred speech and making swallowing more challenging. This difficulty can sometimes lead to a condition known as aspiration pneumonia.
Aspiration pneumonia occurs when food or liquid accidentally enters the airway, leading to lung infections. This emphasizes the importance of seeking professional guidance and support for individuals affected by Parkinson’s. Early intervention and expert care are key to maintaining a high quality of life.
Mood Changes
Depression and anxiety often accompany Parkinson’s, affecting a person’s emotional well-being. These non-motor symptoms can be quite challenging, leading to mood swings, a sense of indifference, and even occasional hallucinations.
This emotional rollercoaster can be as tough as the physical symptoms. It’s essential for patients and their families to be aware of these emotional struggles, as they significantly impact the overall journey with Parkinson’s. An empathetic approach and support are crucial in managing these facets of the condition.
Cognitive Decline
In some cases, people living with Parkinson’s may encounter cognitive challenges, such as difficulties with memory and executive functions. These issues can involve forgetfulness and problems with tasks that require planning and organization.
It’s important to understand that the cognitive aspects of Parkinson’s can be as impactful as the physical symptoms. This is why a comprehensive approach to treatment and support is crucial for maintaining the best possible quality of life.
Living with Parkinson’s: A Guide for Seniors and Caregivers!
Living with Parkinson’s extends beyond physical symptom management. It entails adaptation and embracing life to the fullest.
Navigating this journey involves resilience, a positive outlook, and the pursuit of a fulfilling life. Embracing these principles, individuals with Parkinson’s can find strength and joy in their unique path.
Daily Life Adjustments
You can take steps to make life easier for those living with Parkinson’s disease. Consider simple home improvements such as adding grab bars in the bathroom for extra support, using non-slip mats to prevent falls, or opting for utensils with ergonomic designs for a better grip.
These small changes can greatly enhance daily living. Trust us, these adjustments can go a long way in improving the quality of life for individuals with Parkinson’s.
Tips for Seniors Living with Parkinson’s – Improving Quality of Life
Living with Parkinson’s as a senior can be a challenging journey, but with the right strategies, you can significantly enhance your quality of life. In this guide, we’ll focus on three key tips to help you or your loved ones thrive while managing Parkinson’s.
Establish a Daily Routine

One of the most effective ways to navigate the challenges of Parkinson’s is by creating a daily routine. Having a structured schedule can provide a sense of stability and predictability, reducing stress and anxiety. Here’s how to get started:
- Morning Ritual
- Begin your day with a consistent morning routine that includes gentle exercises, stretching, and a nutritious breakfast.
- This sets a positive tone for the rest of your day.
- Medication Management
- If you’re on medication, establish a specific schedule for taking your doses.
- Use alarms or reminders to ensure you don’t miss any.
- Activity Blocks
- Plan your day with designated time blocks for various activities like exercise, leisure, and rest.
- Be flexible but stick to your schedule as much as possible.
- Evening Wind-Down
- Wind down in the evening with calming activities such as reading or listening to soothing music.
- Aim for a regular bedtime to improve sleep quality.

Utilize Assistive Devices
Incorporating assistive devices into your daily life can make a significant difference. These tools are designed to aid you in various tasks, promoting independence and reducing physical strain. Here are some recommendations:
- Walking Aids
- If mobility is a concern, consider using walking sticks or canes.
- These assistive devices offer support and balance, helping you move with greater ease and confidence.
- Tremor Spoons
- For those with hand tremors, specialized utensils like tremor spoons can make mealtime less frustrating.
- These spoons are designed to minimize spills and improve your dining experience.
- Voice-Activated Technology
- Smart devices like voice-activated assistants can help with tasks like setting reminders, making calls, or controlling the home environment without the need for intricate manual dexterity.
Regular Consultation with Healthcare Professionals
Your journey with Parkinson’s is unique, and it’s crucial to have a reliable healthcare team by your side. Regular consultations with healthcare professionals, including neurologists, physical therapists, and occupational therapists, can help you manage your condition effectively.

These professionals can:
- Adjust your medication as needed.
- Recommend personalized exercise routines to maintain mobility.
- Provide guidance on managing non-motor symptoms like depression and anxiety.
Adopting a structured routine, utilizing assistive devices, and maintaining regular contact with healthcare experts can significantly enhance the quality of life for seniors living with Parkinson’s. By focusing on these tips, you can navigate the challenges of Parkinson’s disease with confidence and improve your overall well-being. Remember, you’re not alone on this journey, and with the right strategies, you can lead a fulfilling life.
Expert Advice for Caregivers
Caring for a loved one with Parkinson’s disease can be an emotional and sometimes challenging journey. As a caregiver, you play a pivotal role in your loved one’s life, providing not only physical assistance but also emotional support. Here, we offer practical advice that combines expertise and empathy to help you navigate this challenging path.
To be an effective caregiver, it’s essential to understand the condition. By educating yourself about the disease, you can better anticipate and address your loved one’s needs.
Patience and Empathy
Parkinson’s can cause a wide range of symptoms, from tremors to mood swings. It’s crucial to approach these challenges with patience and empathy. Your loved one may become frustrated by their limitations, but your understanding can make all the difference.
Seek Professional Guidance
Consider reaching out to healthcare professionals for guidance. They can provide you with valuable insights into managing symptoms, medications, and therapies. Expert advice is just a phone call away, so don’t hesitate to ask for help.
Self-Care
Caring for someone with Parkinson’s can be emotionally and physically demanding. Don’t neglect your own well-being. Taking time for self-care isn’t selfish; it’s a necessity. Whether it’s practising yoga, reading a book, or seeking support from a therapist, remember that you, too, deserve care and attention.
Adapt and Innovate
Parkinson’s symptoms change over time. Be prepared to adapt and innovate. Assistive devices, home modifications, and creative solutions can help maintain your loved one’s independence and improve their quality of life.
Support Networks
You’re not alone on this journey. Seek out support groups where you can connect with other caregivers. Sharing experiences, challenges, and triumphs can be both comforting and empowering.
Advocacy
Advocating for your loved one is a crucial aspect of caregiving. Be their voice when they need assistance navigating the healthcare system or accessing resources. Your advocacy can greatly enhance their quality of care.

Celebrate Small Wins
In the midst of challenges, don’t forget to celebrate the small victories. Whether it’s a good day with fewer symptoms or a joyful moment, these instances are worth cherishing.
Remember Your Importance
Your role as a caregiver is invaluable. In this journey, your role as a caregiver goes beyond the practical—it’s about love, compassion, and being there in every sense of the word. You’re not just a caregiver; you’re a lifeline of support, and your contributions are immeasurable.
Diagnosis and Treatment
Diagnosing Parkinson’s disease is based on a combination of medical history, physical examination, and sometimes imaging tests. While there is no cure for Parkinson’s, several treatment options can help manage its symptoms and improve the patient’s quality of life. These treatments may include:
Medications
In the realm of treating Parkinson’s disease, a variety of medications can effectively address its motor symptoms. Levodopa, often a top choice, is celebrated for its remarkable impact on enhancing mobility. Another option, worth considering in consultation with a healthcare professional, is cannabis.
These medications have the potential to be transformative in improving one’s quality of life. However, it is crucial to emphasize that patients should always consult their physician for a proper prescription and to discuss the most suitable treatment plan tailored to their individual needs.
Levodopa and cannabis are among the therapeutic options that can offer substantial relief, leading to an enhanced quality of life for individuals dealing with Parkinson’s disease.
Physical and Occupational Therapy
Expertise and experience play a pivotal role in enhancing the lives of those with Parkinson’s disease. Through physical and occupational therapy, individuals are empowered to retain their independence and enhance their day-to-day functionality.
These therapies, led by skilled professionals, offer personalized guidance, exercises, and strategies tailored to the unique needs of each patient. By focusing on this specialized care, we foster trust and confidence in the journey toward improved well-being.
Surgical Interventions
In the advanced stages of Parkinson’s, when traditional treatments may no longer suffice, a surgical intervention known as Deep Brain Stimulation (DBS) becomes a viable option.
This procedure involves the implantation of a device that delivers controlled electrical impulses to specific areas of the brain, effectively alleviating symptoms. It’s a testament to medical advancements and a ray of hope for those facing the challenges of advanced Parkinson’s.
Lifestyle Modifications
Maintaining a healthy lifestyle through regular exercise and a balanced diet goes hand in hand with medical treatments to boost your well-being.
This holistic approach not only complements your medical care but also elevates your overall quality of life. The synergy of exercise and nutrition enhances your vitality and ensures a happier, healthier you.
Diet and Nutrition for Parkinson’s Patients
A well-balanced diet is essential to maintain overall health, but for Parkinson’s patients, it’s even more critical. Nutrient-rich foods support brain health, muscle function, and emotional well-being.
Incorporating foods rich in antioxidants, vitamins, and minerals can help combat the oxidative stress that contributes to Parkinson’s progression. Fresh fruits, vegetables, and lean proteins are your allies.
- Protein and Medication Timing
- Balancing protein intake with medication timing is crucial.
- Timing can affect the effectiveness of medication, and a dietitian’s guidance can be invaluable.
- Hydration
- Dehydration can worsen motor symptoms.
- Drinking enough water is essential, but herbal teas and fruit-infused water can make it more enjoyable.
- Fiber and Digestion
- Constipation is a common issue for Parkinson’s patients.
- Fibre-rich foods like whole grains, fruits, and vegetables can help maintain regular digestion.
- Incorporate foods rich in antioxidants, Omega-3 fatty acids, and fibre.
- Personalized Diet Plans
- Individual needs vary.
- Consulting a nutritionist for a personalized diet plan is recommended, considering factors like medication, weight, and personal preferences.
- Supportive Supplements
- Supplements like Coenzyme Q10 and Omega-3 fatty acids have shown promise in managing symptoms.
- Consult with your healthcare team before adding them to your regimen.
- Monitoring Your Diet
- Keeping a food diary helps track what works best for you.
- This data can guide adjustments and ensure your diet aligns with your medication and lifestyle.
- Trust the Experts
- In your journey with Parkinson’s, trust the guidance of healthcare professionals and registered dietitians.
- They possess the knowledge and experience to tailor dietary recommendations to your unique needs.
- Foods to Avoid
- Limit caffeine and sugary foods, which can exacerbate symptoms.

Diet and nutrition are powerful tools in managing Parkinson’s disease. A well-informed approach, tailored to your specific requirements, can enhance your overall well-being and provide the best possible quality of life.
Conclusion
Life with Parkinson’s is a journey of resilience, adaptability, and hope. By harnessing the power of knowledge, community, and technological advancements, seniors and caregivers can navigate this journey with optimism and strength.

Frequently Asked Questions
- What causes Parkinson’s disease?
- There’s no exact known cause, but a combination of genetic and environmental factors may play a role.
- How is Parkinson’s different from other neurological disorders?
- Parkinson’s specifically targets dopamine-producing neurons, leading to its unique set of symptoms.
- Can diet and exercise slow the progression?
- While they can’t halt the disease, a balanced diet and regular exercise can help manage symptoms and improve the quality of life.
- Are there any potential side effects of Parkinson’s medications?
- Yes, but these vary by individual and medication type. Always consult with a healthcare professional about potential side effects.
- How can caregivers help those with Parkinson’s?
- Caregivers can provide physical support, ensure medication routines are followed, and offer emotional companionship.
- Are there any promising treatments on the horizon?
- Research is ongoing, with many potential treatments in the pipeline, including gene therapy and stem cell treatments.
Disclaimer
The content provided on MySeniors.World is for informational purposes only and is not intended as either financial or medical advice. Always consult a qualified professional before making any investment or health-related decisions.
Posts may contain affiliate links, meaning we earn a commission – at no additional cost to you, if you click through and make a purchase. Your support helps us continue providing valuable content.



















